Your gums are like cushions for your teeth; they surround the tooth from its crown to its root in the jaw and help to support a healthy mouth. Looking after your gums is just as important as looking after your teeth, and without routine cleaning gum disease can occur. These are the stages of gum disease:
Fortunately, this can be avoided by attending regular hygiene check-ups at the practice and maintaining a good daily hygiene routine. Brushing between the teeth, flossing and replacing your toothbrush every three months will also benefit your gum health.

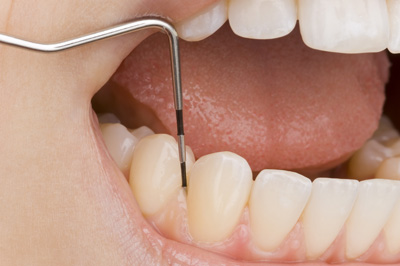
Your periodontist, dentist or dental hygienist diagnose periodontal disease during a periodontal examination. This type of exam should always be part of your regular dental check-up. A periodontal probe (small dental instrument) is gently used to measure the pocket or space between the tooth and the gums.
The depth of a healthy pocket measures three millimetres or less and does not bleed. As periodontal disease progresses, the pockets usually get deeper. The pocket depths, amount of bleeding, inflammation, tooth mobility, etc. are recorded to help make a diagnosis. Click on the links below to get more information on the different types of gum disease.
Brush your teeth twice a day and use a soft bristled toothbrush (safer on your gums) with a fluoride toothpaste. Direct the bristles towards the gum at a 45 degree angle and use a circular motion that moves the brush bristles 'away' from the gums. On the top arch, this would mean you are brushing in a circular direction which is top-down and on the bottom arch, you would be brushing in a bottom-to-top circular motion. Concentrate on 1-2 teeth at a time and repeat the process until all the front and back surfaces of the teeth have been cleaned. Finally, brush the chewing surfaces of the teeth with a horizontal motion. Take care to not speed through brushing, taking at least 2-3 minutes to do a thorough job and don't brush too hard because this can cause gum recession. Replace your toothbrush as soon as the bristles are worn or splayed as they become less effective at that stage. This is usually after about three months.
If you are using an electric toothbrush, angle the bristles at 45 degrees to the gum line. There's no need to scrub. Hold the brush in position and after a few seconds sweep the bristles away from the gum. Repeat around the outer and inner surfaces of all teeth, finishing with the chewing surfaces.

You can clean between your teeth with dental floss, interdental brushes or tape. Dental tape is slightly thicker than floss and many people find it easier to use. Flossing removes plaque and food particles from between your teeth and under the gumline, areas a toothbrush can't reach. You should clean between your teeth at least once a day with floss.
The following suggestions may help:
Break off about 30cm of floss, and wind most of it around one of your middle fingers. Wind the remaining floss around the middle finger of your other hand. As you use the floss, you will take up the used section with this finger.
Hold the floss tightly between your thumb and forefingers, with about an inch of floss between them, leaving no slack. Use a gentle 'rocking' motion to guide the floss between your teeth. Do not jerk the floss or snap the floss into the gums.
When the floss reaches the gumline, curve it into a C-shape against one tooth until you feel resistance.
Hold the floss against the tooth. Wipe the tooth from base to tip two or three times. Repeat on the other side of the gap, along the side of the next tooth.
Don't forget the back of your last tooth.
When flossing, keep to a regular pattern. Start at the top and work from right to left, then move to the bottom and again work from right to left. This way you're less likely to miss any teeth. At first it also helps to look in the mirror. The order in which you brush and floss doesn't matter as long as you do each thoroughly.

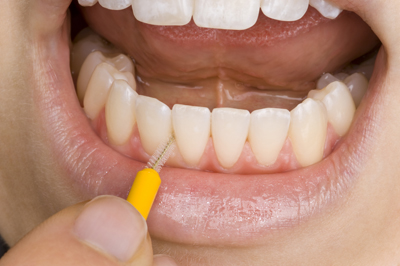
The interdental brush is used to clean in between your teeth. Used at least once daily, it removes plaque and food debris where your toothbrush cannot reach. Turning the brush on insertion will help access. Move the full length of the brush in and out a few times in each space. For spaces at the back of the mouth, bend the brush in a slight curve. This will help you access the more difficult-to-reach areas. Different colour-coded sizes are available to help clean different sized spaces. Do not force the brush in to a space. Guide it in gently or use a smaller size. Change the brush when the filaments are worn.
Use either a fluoride or antiseptic rinse as directed by your periodontist or hygienist.
Twice-daily brushing and regular flossing are excellent for maintenance between dental visits, but a healthy mouth and beautiful smile require routine general and preventive care to stay that way. Our Clinic offers hygiene care that includes regular oral examinations and cleanings.